The Day a Home Visit Saved a Life
In Kathonzweni village, 83-year-old Savethi Mawleu is known for her warm smile, easy laughter, and generous spirit. A mother and grandmother, she lives with one of her children who is battling cancer, while most of her family works in Nairobi. Despite her age and responsibilities, Savethi remains strong and remarkably resilient.
That resilience was tested when Community Health Promoter (CHP) Christine Saina carried out routine household screenings. During her visit, Christine noticed that Savethi’s blood pressure was unusually high and referred her to a local health facility for further assessment. There, facility nurse Marietta Mbithe and Community Health Officer Elizabeth Wambua confirmed that Savethi was living with both hypertension and diabetes.
Since that day, Christine has walked every step of the journey with her ensuring she adheres to medication, counseling her on nutrition, and even accompanying her to distant hospitals for specialized check-ups.
“She checks on me, helps me with my medicine, and teaches me what to eat and what to avoid,” Savethi shares. “Even when I have to go for check-ups far away, like to Kikuyu Hospital for my eye check-up, Saina always accompanies me.”

Christine’s dedication runs deep.
“I am available anytime — day or night,” she says. “There have been times when Savethi called me while I was in Nairobi. I dropped everything and came immediately. And I do this for all my patients, not just her.”
But fate had another twist.
Recently, Christine herself was diagnosed with diabetes — a diagnosis she initially struggled to accept.
“I was in denial at first. It was really hard,” she recalls. “But once I accepted it, I changed my lifestyle. I watch my diet strictly, and I encourage my patients to do the same.”
Elizabeth, who works closely with both of them, witnessed Christine’s transformation.
“I have watched her take this journey. I counselled her personally and helped her reach a place of acceptance,” she says.
Christine believes her diagnosis has deepened her empathy:
“Going through this personally has given me more compassion. I understand what my patients are going through.”

The Bigger Picture: The rise of NCDs in Kenya
Non-communicable diseases (NCDs) are on the rise across Africa, and Kenya is no exception. They now account for 39% of all deaths nationally and 61.7% of hospital deaths, with up to 50% of hospital admissions linked to NCDs. Hypertension and diabetes are among the leading culprits, silently affecting millions and straining health systems.
Without early detection and consistent follow-up, these conditions lead to catastrophic complications—heart disease, kidney failure, blindness—that devastate families and communities. Hypertension affects 1 in 4 adults, yet more than half are unaware of their condition, and are often detected late due to limited screening in rural communities.
Community Health Workers like Christine are critical to reversing this trend. They provide early screening, counselling, follow-ups, nutrition guidance, referrals, and continuous home-based monitoring — services that save lives and prevent complications.
Yet, while CHWs are the backbone of primary healthcare, many of them struggle to access care themselves.
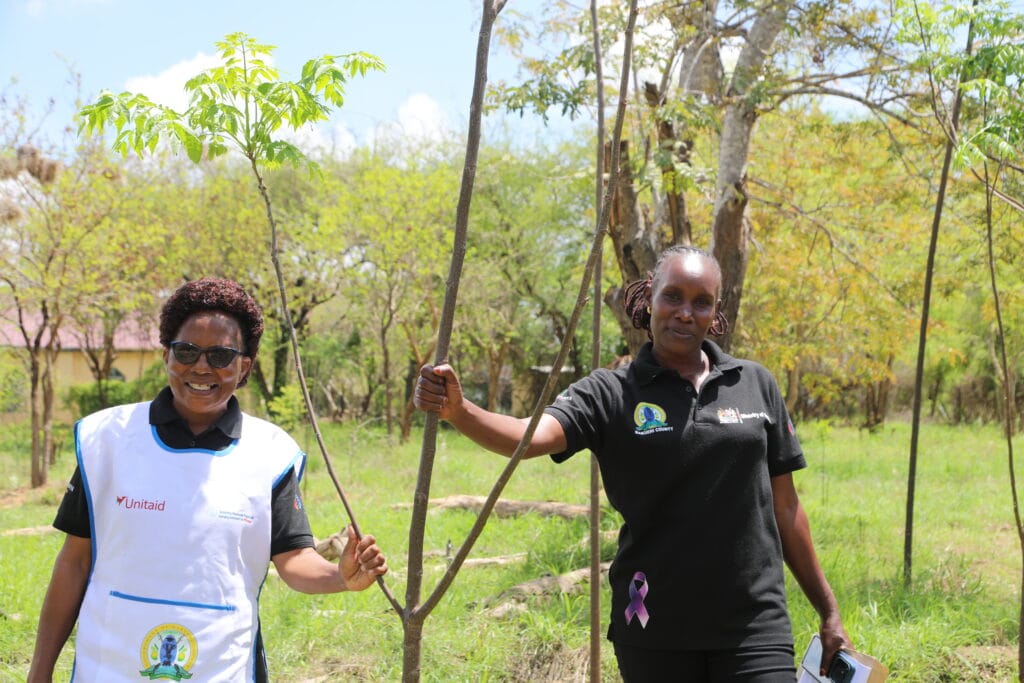
The CHW Paradox — Essential but Underpaid
Across Africa, over 1 million Community Health Workers deliver life-saving care at the household level. Yet, despite their critical role, over 80% of CHWs in Africa are unpaid or inconsistently paid, threatening both their livelihoods and community health outcomes. In Kenya, major progress has been made, and CHWs now receive stipends — but they remain under $40 per month, and sustainability remains a challenge as fiscal pressures tighten.
This economic hardship threatens retention and limits access to care—especially since 70% of CHWs are women, making this a gender equity issue as well.
Despite these hardships, CHWs like Christine continue to show up — every day — delivering results, saving lives, and holding communities together.

FAH’s Work — Building a Future Where CHWs Can Thrive
FAH’s Work — Building a Future Where CHWs Can Thrive
The Financing Alliance for Health (FAH) works at the policy level to institutionalize CHWs in government systems, secure budget allocations, ensuring they are recognized, compensated, and sustainably financed. Beyond policy, FAH strengthens CHWs’ livelihoods through initiatives like the Thrive to Serve Program, which provides:
- Training
- Entrepreneurship and business development skills
- Access to credit and savings groups
- Performance-linked incentives
This holistic approach helps CHWs grow their income, build resilience, and continue delivering quality care to their communities.
Healthy communities begin with empowered community health workers.
Your support helps us strengthen the people who strengthen all of us. Investing in community health is not optional—it’s essential. Every dollar spent on CHWs prevents costly complications and saves lives.




