By Maya Hayakawa
Kenya’s journey toward Universal Health Coverage (UHC) has been defined by bold policies, ambitious frameworks, and a growing consensus that health is both a human right and a national investment. Yet the recent engagement of the Primary Health Care (PHC) Financing Technical Working Group (TWG) underscored a critical truth: policy reforms alone will not deliver results unless they are backed by sustainable, predictable financing. Kenya has done the hard work on policy reform, now the real test is whether we can translate this into sustainable, predictable financing for PHC and community health.
As Financing Alliance for Health, we support the PHC Financing TWG and serve in the Secretariat, providing technical assistance alongside a strong coalition of partners; the Ministry of Health, Council of Governors, County CECs, Chief Officers and Directors Caucus Chairs, HENNET, and other implementing partners. This diversity is intentional: cross-pollination of perspectives is essential if advocacy for PHC financing is to succeed nationally and at county level.

During a recent session, Principal Secretary for Public Health Mary Muthoni challenged conveners to go beyond asking for more money. Her message was clear: While PHC financing remains fragmented, Kenya must improve efficiency, expand fiscal space, and pursue innovative financing models — including blended finance, results-based approaches, smarter pooling, and strategic purchasing — to maximize the impact of every shilling. Health is not a cost to be managed; it is an investment to be nurtured. “Efficiency is our greatest resource” she said, “We must maximize the impact of existing resources while progressively strengthening domestic resources”.

Kenya's Vision for Health
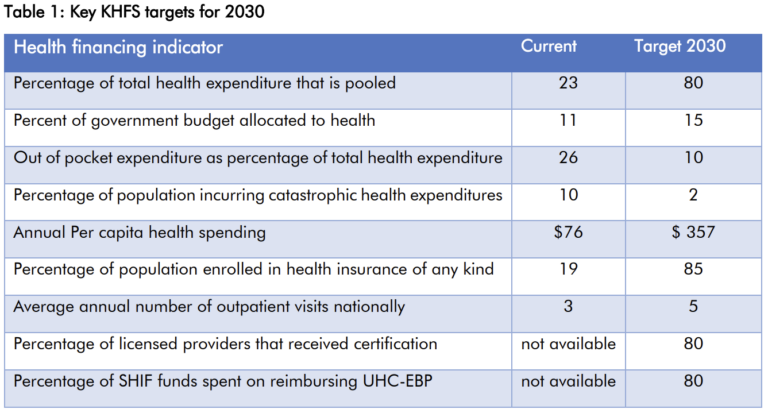
Kenya’s Vision 2030 and its Vision for Health 2030 place primary healthcare at the center of national development, recognizing that a healthy, skilled workforce is essential to drive economic growth. The national government has also set ambitious targets — including over 80% insurance coverage for the population and a reduction in catastrophic health spending to 2% — although progress toward these goals continues to lag.

Source: Ministry of Health Kenya, Kenya Health Financing Strategy 2020-2030
Despite progressive policies and institutions — including the Primary Health Care Act, Social Health Authority Act, Facility Improvement Financing Act, and Digital Health Act — health investment remains insufficient. Estimates from Kenya National Health Accounts 2018/19 show per capita health spending at US$76, below the WHO’s recommended US$86 for essential health services. Moreover, Kenya has yet to reach the 15% budget allocation target set by the Abuja Declaration, with the health share currently sitting at around 11%.
Source: Ministry of Health Kenya, Kenya Health Financing Strategy 2020-2030
Government financing accounts for nearly half of total health expenditure, but it has not risen fast enough to offset declining donor support or reduce households’ reliance on out-of-pocket spending. Although out-of-pocket costs have fallen over the past decades, they remain high and stagnant in recent years.
With these landmark health financing reforms in place, the financing question becomes even sharper:
- If we can progressively expand financing for highly specialized curative services, can we not demonstrate the same ambition for PHC?
- How do we continuously advocate for PHC budget growth with the same discipline and consistency as sectors like defense or infrastructure?
- How do we strengthen allocative efficiency so today’s investments translate into long-term population health and fiscal sustainability?
Director General for Health Dr. Patrick Amoth reminded the TWG of PHC’s original ethos: inclusive, people-centered, preventive, and equitable care. While curative care has dominated funding, evidence shows that investments in PHC yield high returns — both in health outcomes and economic benefits — when financed effectively.
The TWG’s work is not just technical; it is strategic. To secure Kenya’s health future, we must advocate with discipline, measure performance transparently, and document gains rigorously. PHC must be financed like a national priority, not a residual afterthought.
If Kenya is serious about sovereignty, resilience, and equity, we must fund our health system starting at the primary care level — with communities at the center.




