Community health is a critical foundation for achieving Universal Health Coverage (UHC) in Kenya, delivering essential services to households, especially in underserved areas. As the first point of contact with the health system, Community Health Workers (CHWs) play a vital role in prevention, health promotion, and linkage to care. However, the effectiveness of community health systems depends not just on their existence, but on how well they function. Measuring the maturity of these systems allows stakeholders to assess performance across key components, such as governance, financing, training, and data use and identify actionable gaps. This ensures that community health is not only expanded but strengthened to sustainably support Kenya’s health goals.
A Participatory Approach to Evaluating Systems Maturity
The assessment employed a participatory approach that actively engaged stakeholders from the Ministry of Health (both national, county levels and community health promoters’ representatives) and implementing partners. Using the Community Health Systems Maturity Assessment Tool, the process combines targeted training, open dialogue, and collaborative group scoring based on a four-level scale, from non-functional to highly functional. This approach ensured broad input, transparency, and alignment with national priorities. The tool assessed nine critical pillars of the health system: leadership and governance, planning, financing, CHW remuneration, pre- and in-service training, supportive supervision, health information systems and M&E, commodity supply, and community engagement. This inclusive methodology not only enhanced the quality of the process but also fostered collective ownership of the assessment outcomes and recommendations.
Where Are We Now? Uncovering Gaps That Undermine Impact
Kenya’s community-health platform already rests on solid foundations, national policies, the new Primary Health Care (PHC) Act, a costed strategy, and a fully deployed electronic community health information system (eCHIS) give the country a head-start toward Universal Health Coverage. But the maturity baseline shows that every domain still sits at only partially or moderately functional, while the 2027 goal is “highly functional. Below is a headline view of the key gaps that must be closed across each domain to bridge that baseline-to-target divide:
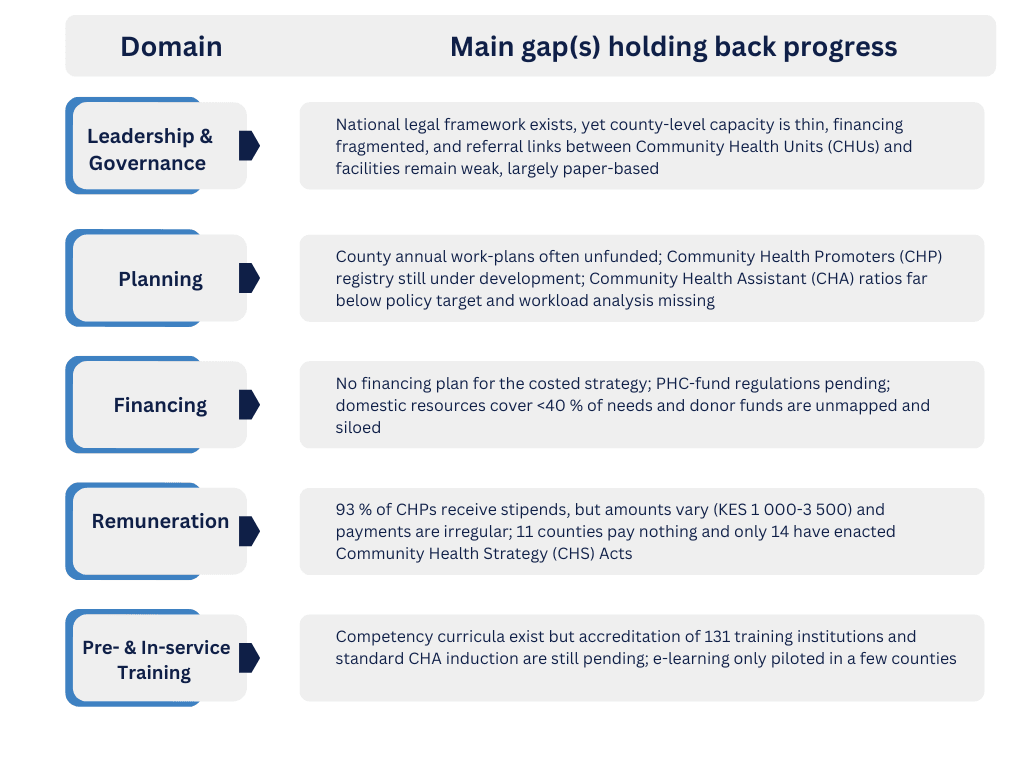
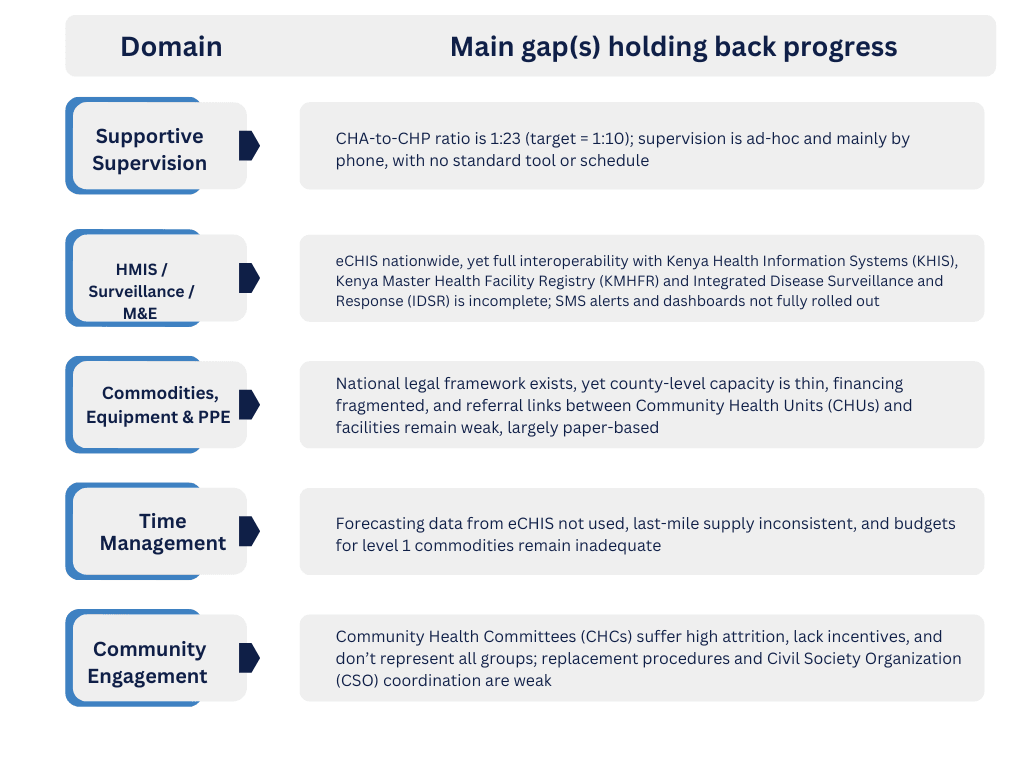
Turning Insights into Actions. The Bottom Line
Kenya’s path from a “solid but uneven” community health foundation to a truly “highly functional” system by 2027 depends on how well we act on what this maturity assessment has revealed. Bridging the gaps won’t happen by chance; it requires deliberate, targeted investments and stronger alignment across national and county governments, partners, and communities. This will be achieved by strengthening local capacity, securing dedicated financing, harmonizing CHP stipends, and standardizing training and supervision. Integration of digital systems, reliable supply chains, and revitalized community engagement structures like CHCs are also key. With coordinated action and sustained commitment, Kenya can build a resilient, equitable community health system that truly delivers for every household.
Building Together: A Coordinated Roadmap for Community Health Strengthening
This maturity assessment was made possible through strong collaboration between the Division of Community Health and a diverse coalition of technical and funding partners. Financing Alliance for Health (FAH), through Strategic Initiative Funding from the Global Fund, continues to support the national government with technical assistance, system strengthening, and efforts to mobilize domestic investment in community health. The Community Health Units for Universal Health Coverage (CH4UHC) ecosystem, and county governments have brought critical expertise across digital health, training, supervision, and financing. Together, these actors are aligning efforts to advance Kenya’s vision of a highly functional and sustainable community health system.
To guide this transformation, the report outlines a clear action plan for the next 12 months and beyond. Priorities include finalizing PHC Act regulations, standardizing training, harmonizing stipend payments, improving supervision systems, and integrating digital health tools. A comprehensive technical assistance plan underpins these actions, ensuring a coordinated, evidence-informed pathway to results.
Looking Ahead. Turning Commitments into Action
Achieving a highly functional community health system by 2027 is within reach but only if we act decisively. The roadmap is clear. What’s needed now is a collective follow-through. We urge national and county governments to prioritize and fund the reforms laid out in the maturity assessment. Parliament must play its role in enacting enabling legislation and holding the system accountable. Development partners should align their investments with the national plan, supporting long-term systems rather than short-term fixes.
This is the moment to move from commitment to implementation, so that every household in Kenya can rely on a strong, well-supported community health system.
The time to act is now!
About the Authors

Wendy Wakhusama
Wendy Wakhusama is a seasoned partnerships, fundraising, and strategic communications professional with over a decade of experience mobilizing resources and building transformative collaborations across the public, private, and philanthropic sectors.

Geredine Kandie
is a Health Financing Technical Advisor at the Financing Alliance for Health, a change agent who is passionate about system strengthening with a focus on primary health care. A champion of everyday heroes transforming lives in our communities




